Parasitic STIs
Overview
About Parasitic STIs
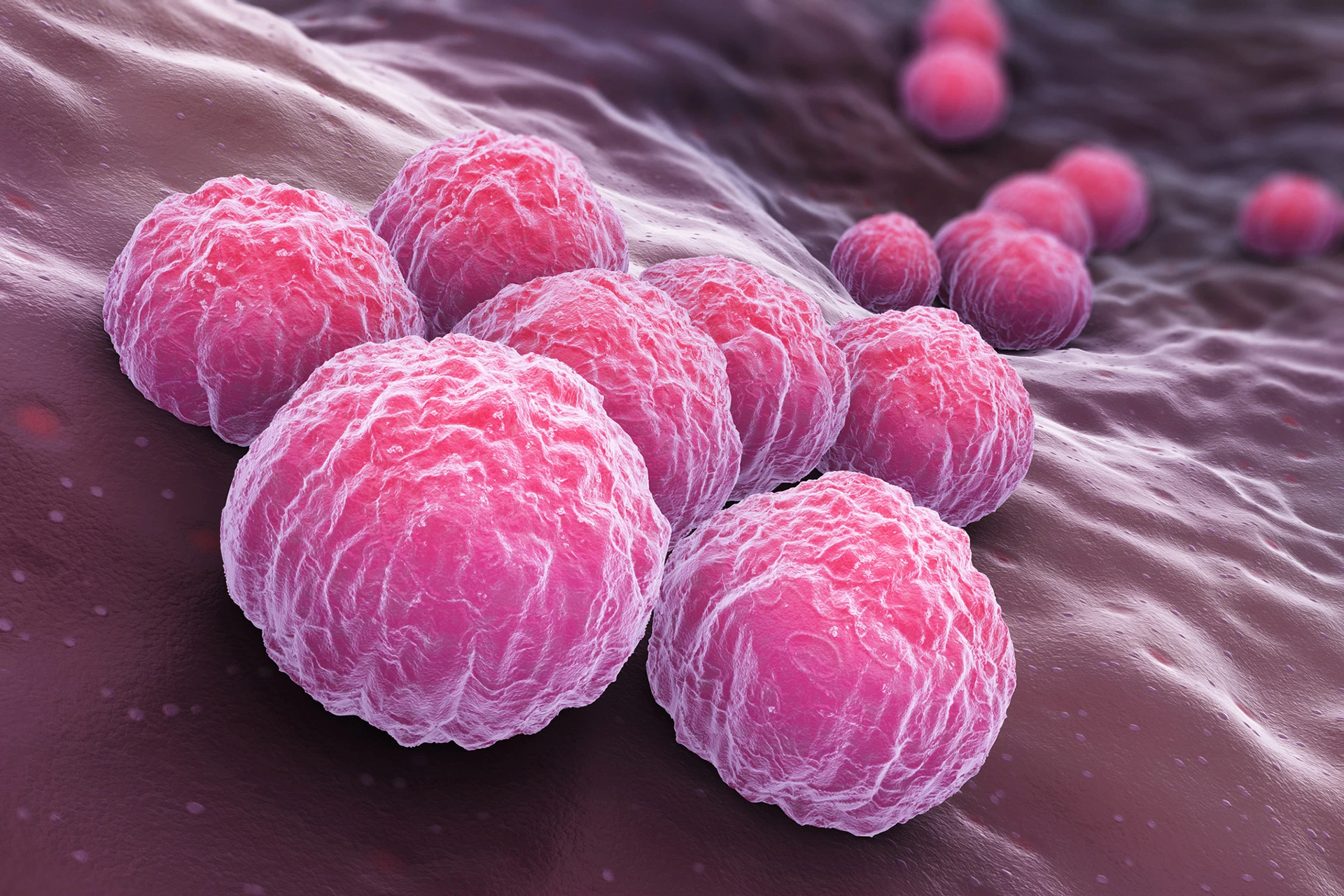
Some infections—such as trichomoniasis (“trich”), scabies, pubic lice, and certain intestinal illnesses—are caused by parasites. These organisms depend on a host to survive, often causing harm in the process.
Some parasites live inside the body. For example, trich and intestinal infections (like giardiasis or amebiasis) grow within the digestive or reproductive systems. Others, like scabies and pubic lice, are external.
These infections may have short- and long-term effects. Understanding this can empower individuals to make the best decisions for their health.
Trichomoniasis
Trich is the most common non-viral STI. It is caused by a microscopic single-celled organism. Symptoms include vaginal discharge, itching, pain with sex, or discomfort with urination. Most people have no symptoms, but they can still spread the infection to others. Trich should be treated with antibiotics, as untreated trich increases the risk of HIV, cervical cancer, pelvic inflammatory disease (PID), or birth complications.
Pediculosis Pubis
Pediculosis pubis (also known as “pubic lice” or “crabs”) are small (<1mm) crab appearing lice that infest the pubic hairs and other coarse hairs. They spread by intimate contact. An infestation is diagnosed by visualization of the crabs. Pubic lice is treated with over the counter or prescription medications, and nits (eggs) are removed with a fine tooth comb. Household contacts and sexual partners should also be treated, and all linens should be washed and dried on high heat cycles.
Scabies
Scabies is caused by small mites which burrow beneath the surface of the skin and cause a pimple like rash and itching. Visualization of the rash and evidence of the mites is used to diagnose this infestation. It is treated with prescription topical or oral medication. Household contacts and sexual partners should also be treated and linens washed and dried with high heat.
Enteric Infections
Some intestinal infections, such as giardiasis or amebiasis, can spread sexually due to contact with fecal matter. This type of transmission is most common amongst men who have sex with men (MSM). Symptoms include diarrhea, bloating, or nausea. Less commonly these infections can spread to other body organs, causing serious complications.
Trichomoniasis
Overview
Trichomoniasis (Trich) is the most common non-viral STI. When symptomatic, it causes genital inflammation, itching, discomfort, or odorous discharge.
Prevalence
Trichomoniasis is the most common non-viral STI. It affects about 2.8 million people in the United States (CDC, 2022). It is more common in women than men.
Transmission
Trich spreads during penile-vaginal sex or vaginal-vaginal sex (CDC, 2022 & McCance and Huether 2019).It rarely spreads among men who have sex with men (MSM). Trichomonas can survive for very short periods of time outside the body — so spread through contact with contaminated objects such as sex toys is possible. It can also spread from mother to newborn during childbirth.
Symptoms
70-85% of people with trich have no symptoms. Symptoms in women include abnormal vaginal discharge (copious, odorous), discomfort with sex or urination, or genital itching or redness. Symptoms are often more prevalent during menses. Symptoms in men are rarer, and include mild itching, discharge, or discomfort with urination or ejaculation.
Complications
Trich is associated with a higher risk of cervical cancer, HIV, and pelvic inflammatory disease (PID). PID is an infection of the reproductive tract in women that can cause permanent damage and scarring — increasing the risk of infertility and ectopic pregnancy (pregnancy outside of the womb).
In pregnant women, it increases the risk of preterm birth, low birth weight, or premature rupture of membranes.
Diagnosis
Trich is diagnosed by cervical, vaginal, or penile swab, or by urine sample.
Treatment
Oral antibiotic medication is typically used to treat trich. Sexual partners should also be treated, even if they have no symptoms. The CDC recommends follow up testing 3 months after treatment, as reinfection is common.
Prevention
Consistent and correct use of condoms reduces the risk of acquiring STIs (such as trich) by about 60% (Crosby et al., 2012). Male circumcision also reduces the risk of acquiring trich.
Sex outside of a long-term faithful relationship increases the risk for acquiring sexually transmitted infections. Before engaging in sexual activity with a new partner, have an open and honest conversation about past STIs, and consider getting tested for STIs. Many STIs have no symptoms but have lasting consequences.
Pediculosis Pubis (Pubic Lice)
Overview
Pediculosis pubis (also known as “pubic lice” or “crabs”) are small (<1mm) crab appearing lice that infest the pubic hairs and other coarse hairs. They spread by intimate contact.
Diagnosis
An infestation is diagnosed by visualization of the crabs.
Treatment
Pubic lice is treated with over-the-counter or prescription medications, and nits (eggs) are removed with a fine tooth comb. Household contacts and sexual partners should also be treated, and all linens should be washed and dried on high heat cycles.
Scabies
Overview
Scabies is caused by small mites which burrow beneath the surface of the skin and cause a pimple like rash and itching.
Diagnosis
Visualization of the rash and evidence of the mites is used to diagnose this infestation.
Treatment
It is treated with prescription topical or oral medication. Household contacts and sexual partners should also be treated and linens washed and dried with high heat.
Enteric Infections
Overview
Some intestinal infections, such as giardiasis or amebiasis, can spread sexually due to contact with fecal matter. This type of transmission is most common amongst men who have sex with men (MSM).
Symptoms
Symptoms include diarrhea, bloating, or nausea. Less commonly these infections can spread to other body organs, causing serious complications.
Last updated on May 7, 2026
In the News


References
Centers for Disease Control and Prevention. (2024, June 4). About pubic “crab” lice. https://www.cdc.gov/lice/about/pubic-lice.html
Centers for Disease Control and Prevention. (2024, June 6). Pthiriasis. https://www.cdc.gov/dpdx/pthiriasis/index.html
Centers for Disease Control and Prevention. (2024, September 9). About scabies. https://www.cdc.gov/scabies/about/index.html
Fernández-Huerta, M., Zarzuela, F., Barberá, M. J., Arando, M., Esperalba, J., Rodríguez, V., … & Sulleiro, E. (2019). Sexual transmission of intestinal parasites and other enteric pathogens among men who have sex with men presenting gastrointestinal symptoms in an STI unit in Barcelona, Spain: a cross-sectional study. The American journal of tropical medicine and hygiene, 101(6), 1388.
McNeil, C. J., Kirkcaldy, R. D., & Workowski, K. (2022). Enteric infections in men who have sex with men. Clinical Infectious Diseases, 74(Supplement_2), S169-S178.
McCance, K.L., & Huether, S.E. (2019). Sexually transmitted infections. In V.L. Brashers & N.S. Rote (Eds.), Pathophysiology: The biologic basis for disease in adults and children (pp 883-885, 1514). Elsevier.
Trich References
Centers for Disease Control and Prevention. (2022, September 21). Trichomoniasis. https://www.cdc.gov/std/treatment-guidelines/trichomoniasis.htm
Crosby, R. A., Charnigo, R. A., Weathers, C., Caliendo, A. M., & Shrier, L. A. (2012). Condom effectiveness against non-viral sexually transmitted infections: a prospective study using electronic daily diaries. Sexually transmitted infections, 88(7), 484–489. https://doi.org/10.1136/sextrans-2012-050618
Kawssan, A., Chawiche, C., Shamas, Z., & Hamdar, H. (2024). Non-sexual transmission of sexually transmitted diseases in women. Journal of Medical Research and Reviews, 3(1), 17-22.
McCance, K.L., & Huether, S.E. (2019). Sexually transmitted infections. In V.L. Brashers & N.S. Rote (Eds.), Pathophysiology: The biologic basis for disease in adults and children (pp 883-885, 1514). Elsevier.
Van Gerwen, O. T., Opsteen, S. A., Graves, K. J., & Muzny, C. A. (2023). Trichomoniasis. Infectious disease clinics of North America, 37(2), 245.